

The gut may seem distant from the main source of action in chronic fatigue syndrome (ME/CFS) and fibromyalgia (FM) but more and more studies suggest that gut problems can affect everything from the cardiovascular system to the immune system to the brain.

The gut is far more than the seat of digestion.
The gut is far more than the seat of digestion. It has its own special nervous system (the enteric system) which produces hormones, neurotransmitters, and immune factors. Seventy percent of the cells that produce inflammation are associated with gut tissues. Gut dysbiosis and gut inflammatory factors have been linked to everything from arthritis to major cardiovascular events to anxiety to the amyloid plaques found in Alzheimer’s disease. Reduced gut biodiversity has even been associated with poor sleep.
Numerous studies have uncovered gut issues in ME/CFS and FM. At least five studies, including one published this year, have found evidence of gut dysbiosis (harmful gut bacteria) in ME/CFS, and several have pointed a finger at the gut microbiome in FM. Reduced gut biodiversity – found in both ME/CFS and FM – has been associated with chronic widespread pain as well. One hypothesis proposes that a sort of “dysbiotic march” begins with irritable bowel-like syndromes and ends up with fibromyalgia and/or ME/CFS.
While we don’t know how much of a problem the gut causes in ME/CFS and FM it’s clearly a player. Given that t’s no surprise to learn that it’s also a player in Gulf War Illness (GWI). In fact, GWI gut researchers are plowing ahead and uncovering new treatment possibilities that may help restore the gut to health in ME/CFS and FM as well.
A Gut-Brain Connection in Gulf War Illness
Saurabh Chatterjee in South Carolina has a knack for publishing intriguing papers. In 2017, Chatterjee used a Gulf War Illness (GWI) animal model to show that the combination of an anti-nerve agent (pyridostigmine bromide), an insecticide (permethrin) – plus a nice dose of stress (corticosterone) as a mixer – did a number on the guts of GWI mice.
As their healthy gut flora tanked, their nasty gut flora (Firmicutes and others) pried apart the junctions in their gut lining allowing bad bacteria to spill into their bloodstream. That, not surprisingly, agitated the immune system, which responded with a pro-inflammatory response (toll-like receptor 4 (TLR4)) that reached all the way to the brain. Given the systemic response that had originated, apparently, in the gut, the authors suggested boosting gut health of GWI patients with antibiotics like minocycline and probiotics.
A small chronic fatigue syndrome (ME/CFS) study found that a different stressor – exercise – also increased Firmicutes bacteria. Given the small size of the study, the authors were surprised at how clearly the differences in the gut flora jumped out. While exercise dramatically altered the gut flora in people with ME/CFS it affected the gut flora of healthy controls hardly at all.
Much as did Chatterjee et. al., the authors noted that gut flora manipulation, including probiotics, prebiotics, dietary fiber, and fecal microbiota transplantation, was a possibility as they’ve proven helpful in “other chronic, inflammatory, non-communicable diseases.”
Antivirals for the Gut?
Chatterjee’s next study, “Gut DNA Virome Diversity and Its Association with Host Bacteria Regulate Inflammatory Phenotype and Neuronal Immunotoxicity in Experimental Gulf War Illness“ (Nancy Klimas was a co-author), attempted to explain how a chemical exposure, an anti-nerve agent, and stress had impacted the gut of all places. It opened an entirely new window on what might be happening in GWI, as well as chronic fatigue syndrome (ME/CFS) and other diseases.
The study found that viruses in the gut – known as bacteriophages – thrived on the chemicals the mice had been exposed to. While bacteriophages haven’t received nearly the study that gut bacteria have, they’re considered the great regulators of our gut flora.
Since the gut virome appeared to be the core player in the gut dysbiosis found, Chatterjee turned not to an antibiotic but to a broad-spectrum antiviral called Ribavirin. Ribavirin is mostly used to treat hepatitis C and viral hemorrhagic fever but, in this case, not only did it return the gut virome to health, but it also stopped the leaky gut and reduced the inflammation in the brain…
The authors, one of whom was Nancy Klimas, suggested that antivirals like Ribavirin, by themselves or in combinations with “complementary and alternative compounds and probiotics”, might “form the basis of a novel treatment strategy for GWI and similar disorders.”
Just last week, Chatterjee and his South Carolina team (and Nancy Klimas) took a different crack at restoring the wounded microbiomes of their unfortunate GWI mice. This time they used something much more accessible than an antiviral – an herbal supplement called andrographolide.
Andrographolide
Andrographolide (AG) is not just any herb. In fact, it’s not an herb at all. It’s a chemical compound that comes from an herb called Andrographis paniculata found in India, China, and Australia. Andrographolide is used extensively in Chinese and Indian medicine. While its anti-inflammatory, antibacterial, antivirus, antitumor, and cardiovascular protecting properties have excited many, its low bioavailability has been a problem. That problem has prompted much work to create more potent derivatives.
AG has been well studied, leaving the medical literature studded with reviews. Over the past couple of decades, hundreds of derivatives have been developed and bioavailability has been improved. A 2020 review of the many efforts made to improve the usefulness of this unique compound demonstrated how active the andrographolide field is. There’s clearly still work to be done, though. While lauding the “ancient mighty herb” – and its perhaps mighty compound – a 2018 Chinese review asserted that better forms are needed.
In its current form andrographolide is still pretty potent. A 2017 review of andrographolide’s antiviral and immune properties reported that it does something that might be quite helpful in ME/CFS – boosts cytotoxic T cell and natural killer (NK) cell functioning. Two more recent reviews lauded it for its antioxidant, anti-inflammatory properties, and neuroprotective properties.
To wit – andrographolide has generated a lot of interest. This is the first time, though, this “wonder compound” has shown up in Gulf War Illness, ME/CFS, or fibromyalgia. (Quite a few studies have been focused on its potential effects on the coronavirus, though).
Chatterjee’s latest study “Andrographolide Attenuates Gut-Brain-Axis Associated Pathology in Gulf War Illness by Modulating Bacteriome-Virome Associated Inflammation and Microglia-Neuron Proinflammatory Crosstalk“, was a mouthful – and for good reason – it was quite a complex effort.
The authors (which again included Nancy Klimas) found that AG restored the mouse microflora, and improved it by increasing the abundance of two bacteria species (Lachnospiraceae, Akkermansia, Bifidobacterium), which are both “immensely helpful in maintaining robust gut and immune health”.
Significant decreases occurred in two virome families (Siphoviridae, Myoviridae) known to negatively impact gut health. As that happened, the leaky gut tightened up, and inflammatory cytokine levels in the blood decreased. In a result they called “very significant”, microglial activation – potentially the source of so much misery – decreased as well. Some evidence suggested that that other crucial barrier – the blood-brain barrier – tightened up as well.
Their examination of the “microglial secretome”, via harvesting the microglial conditioned medium (MCM), found that AG reduced the phosphorylation of the tau protein in the brain. Tau phosphorylation produces “neurofibrillary tangles” and “neuropil threads” that interfere with nervous system functioning. These tangles and threads have been implicated in the progression of Alzheimer’s disease.
Increased levels of phosphorylated tau have not been found in GWI (it doesn’t appear that anyone has looked for them), but significantly elevated levels of Tau antibodies have been found – and suggest phosphorylated tau could be present.
It was remarkable to see this plant compound possibly reverse levels of phosphorylated tau, rebalance the gut flora, heal the gut lining, and reduce inflammation in the body and neuroinflammation in the brain. Sometimes we forget what a potent source of effective drugs plants are. While more and more drugs are being synthesized in the lab, more than 60% of clinically approved anticancer drugs come from medicinal plants.
In conclusion, the authors stated that the:
“AG treatment mitigated the Gut–Brain-Axis associated pathology in GWI and may be considered as a potential therapeutic avenue for the much-needed bench to bedside strategies in GWI.”
Placebo-controlled trials in humans will hopefully be next. AG is readily available in supplement form in the U.S.and WebMD has prepared a section on it. Check out several reviews of the best AG supplement to take.
The GWI mouse-gut story doesn’t end here. Ample Department of Defense funding has produced an integrated and well-organized effort that has clearly has helped the field take rapid steps towards human trials. Another nutraceutical that I’ve never heard of also produced some nice gut harmonization in a GWI mouse.
Sparstolonin B (SsnB)
A study (with Nancy Klimas as a co-author) found that Sparstolonin B (SsnB) – another compound with a difficult name – which was derived from a Chinese herb, increased the abundance of butyrogenic bacteria, helped tighten up the crucial junctions lining the gut, and reduced inflammation and neuroinflammation. Sparstolonin B (SsnB), which has also recieved quite a bit of study, interestingly, appears to be able to protect the blood vessels from harm – a possibly key need in ME/CFS.
Note that similarly reduced levels of gut-protecting butyrogenic bacteria have been found in both ME/CFS and fibromyalgia (FM).
The Gist
- The gut is far more than the seat of digestion. Studies indicate that the gut affects many systems and plays a role in many diseases including chronic pain disorders like fibromyalgia, cardiovascular diseases, and central nervous system diseases like Alzheimer’s.
- Numerous studies have implicated bad gut flora in ME/CFS and fibromyalgia. Others have linked reduced gut diversity to chronic pain and problems with sleep.
- Behind substantial federal support, Gulf War Illness (GWI) studies have been plowing new ground. A 2019 paper showed that the gut virome was severely disturbed in a GWI mouse model, and that an antiviral called Ribivarin was able to restore the gut to health.
- In the latest study, South Carolina researchers found that a plant compound called andrographolide not only restored the gut bacteria to health, it also readjusted the gut virome, repaired leaky gut, and knocked down inflammation in the body and brain. It even appeared to reduce the phosphorylation of the tau protein which produces threads and tangles which have been implicated in Alzheimer’s.
- In another study, another plant compound called Sparstolonin B (SsnB) produced much the same effects.
- The Gulf War researchers are benefitting from a well-funded and organized approach to GWI that is spinning off clinical trials right and left. ME/CFS has never received that kind of approach but long COVID surely will. At some point, we will likely be awash in long COVID treatment trials.
- While mice are not humans, disease mouse models can provide crucial insights into diseases and can pave the way for human trials.
- Meanwhile, GWI research is uncovering treatment possibilities that may benefit it and ME/CFS and FM as well.
Piggybacking Off the GWI Field
How nice it must be to have funding – and an animal model. Unfortunately, the ME/CFS field has never received the kind of support that would allow it to take an integrated, multidisciplinary stab at the disease and produce clinical trials. Walter Koroshetz warned that, based on his experience, it was too early for the NIH to fund clinical trials, as unsuccessful trials can sink future efforts. He may be right, but it’s clear that the NIH’s refusal to adequately fund and support ME/CFS is the driving force behind that situation.
While that fact will, no doubt, continue to rankle for quite a while, Congress’s willingness to send over a billion dollars to the NIH to study long COVID means that, at some point, we should have long COVID treatment trials coming out of our ears.
In any case, it’s clear that the generous GWI funding the DOD is providing is potentially having some nice spillover effects for ME/CFS – including new treatment possibilities.
Conclusion
These are mouse studies that may or may not translate to humans, but as mouse studies are often the first step to human drug trials, there’s clearly enough overlap between humans and mice for researchers to use them, again and again, to suss out possibilities.
The studies illuminated once again, what a powerful influence the gut – in particular, a leaky gut – can have on both the body and the brain. While one might have expected the combination of a stressor, an anti-nerve agent, and an insecticide to give the central nervous system a good whack, it was surprising to see how much it also affected the gut. It now appears, as well, that the gut microbiome is much more than about the gut bacteria – the gut virome must be studied as well. In fact, if the gut virome is the great gut flora regulator, it may take central place at some point.
With similar gut findings showing up in ME/CFS and FM, and the GWI field producing new treatment possibilities for the ME/CFS and FM fields to mull over, the GWI field is clearly a field to keep an eye on. Nancy Klimas, by the way, is beginning a clinical trial using a novel probiotic that’s found only in Europe.

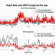





Lipkin found elevated levels of the common pesticide Round-up in the guts of people with ME/CFS compared to controls. I personally grew up in a wine region that was heavily sprayed.
Presumably most people aren’t exposed to pyridostigime bromide but perhaps some types of virus have anticholinergic effects?
Stress is pretty universal, as are genetic weak points (methylation issues, etc), so maybe the recipe for GWI is somewhat similar to a subtype of ME/CFS, except swapping PB for a virus.
Another instance of a pesticide impacting the gut. Who knew?
My gut has always been a weak point for me. When I became ill in 2004 I was living next to a corn field. We had asked the farmers if they sprayed with pesticides and they said no. After I became ill we found out that technically they didn’t spray… they hired someone else to. I think it was one of the factors that contributed to my illness.
My gut is the only possible weak link dating back to my childhood that I can think of. Nothing dramatic but I remember quite a few messy bowels.
Hi Cort,
Its Chris to whom you suggested blogging recently.
This is a very well-done article.
If you dont recall, my elderly friend, the impetus for my research reviewing, has fibro, cfs, vision problems, Raynaud’s phenomenon and more. She has celiac disease and casein (milk) allergy.
When she was 6 months she contracted whooping cough and because it wouldnt leave her they gave her massive amounts (at least in total) of tetracycline. So I dont see how her gut biome could have escaped disruption. Hing Kong Flu at 16, and aldo contracted H1N1 when that came around.
So it was very helpful to stop eating gluten because that would just knock her down. According to Anthony Fasano, possibly all autoimmunity starts with leaky gut and gluten triggers the release of zonulin which, as you described it, tears apart what are supposed to be TJ (tight junctions) of the one-cell thick outer lining of the intestine.
But you triggered a very important thought: Yes, of course the brain would suffer inflammation and maybe even become (hyper) sensitized to pain if the BBB were compromised while a new antibody were making the rounds. Thats how I see damage from pandemics.
But if not only zonulin but also the compound you mentioned can loosen the tight junctions of the intestine, then, call me an amateur, but I dont see why they wouldnt both do that to the BBB once they “escape”.
Fasano mentioned that zonulin is produced in several non-intestine parts of the body. The way I interpret that is that , ok, the gluten provokes zonulin and the zonulin opens the leaking gut…. but that means that gluten can travel throughout the bloodstream– and provoke zonin elsewhere.
And likewise might the junction-loosening compound that you speak of circulate.
As I recall, about 80 percent of the immune system resides in the gut. And as Ron mentioned, somewhere close to 80 percent of serotonin resides there as well. Its a good location from which to mobilize serotonin.
I dont see it as at all surprising that the pesticides harm the intestine because where else is the liver supposed to perform its work? The body will send it there. If it could just make uric acid from the pesticide then it would, but these are chemicals the body was not designed to encounter.
Lastly, During covid research it was reported that those who already had dysbiosis tended to have much worse outcomes from covid. There was some question: did the leaky gut help covid? Or did covid cause leaky gut.
But the prescription is the same: fix your gut. Its never too late.
There has also been a recent research concensus the ladt few months that the worst part of covid is vascular damage. Veins, arteries, capillaries. The lungs are first, of course, with their many ACE-2 receptors. But I have learned that ACE-2 receptors are throughout the circulatory system endothelial cells, they are in the kidneys, pancreas, liver, …. basically in non-skeletal muscle, or “smooth muscle” and it makes perfect sense that once there is widespread vascular damage, lingering widespread pain is a likley outcome.
My fibromyalgia started with a very severe bout of IBS that lasted 6 months. Prior to that I had bladder and pelvic pain.
After such a long ordeal my digestive system had really desensitized and other problems showed up too. Back pain, headache, widespread muscle pain.
Hi Cort, on another topic, to whom should I send a report of my success with taking high-dose Thiamine (B-1)? I have been on it for about a month, I am up to 3 mg per day, and while I still have some bad days, the number of good days has increased significantly. I recently had 11 days of feeling better than I can remember since the ME/CFS began. I actually have been having energy and a feeling of ambition to do things I wouldn’t have even tried in several years. The nausea and gut problems have decreased in frequency, my foggy brain is noticeably better and the vertigo is better. A lot of questions still need to be answered but I am feeling so much better on good days and the number of good days have increased.
Should read: I am up to 300 mg of Thiamine.*
debsw, you may already know this but it’s pretty well accepted that Roundup is the culprit in all the gluten intolerance in the U.S. While I am gluten intolerant since having ME/CFS, I seem to be able to eat baked goods from Europe which don’t cause the IBS symptoms when I eat US wheat based goods
Roundup decimates and disrupts the microbiome, gluten is not adequately digested and causes the intolerance problems.
It simply casuistry to say that Glyphosate is not toxic to humans, and it *is* definitely toxic to that foundation of nutrition and health, the gut microbiome.
Anyone considering an FMT, talk to your doctor, but here are a few things I remember about it all:
1. Get your microbiome scanned. This would probably be part of the protocol followed by your doctor these days. If not, there are laboratories of various descriptions that do it. But they are not everywhere. The first time I did an FMT, the American Gut Project was the only way to get any microbiome information. It is better than nothing (and in my case, enough to provide supporting evidence for significant gut dysbiosis). The most recent time I thought about doing another FMT, there is a much better private company that now provides a far more detailed microbiome scanning service, and it showed things were within acceptable bounds. So I didn’t proceed with another FMT.
2. Get your own donor:
2a Young, same sex
2b The fitter the better (athletes have different microbiomes)
2c Make sure you know them well enough to exclude risks (recreational drugs, STDs, poor diet, mental health, work/environmental exposures etc).
2d Not a relative
3. Get your donor screened according to the best testing protocols. Your general doctor or gastroenterologist should be able to help with this, otherwise there are a few different protocols. No doubt now including Coronavirus screening.
4. There is always a cleaning out process before the first FMT (obviously, not the subsequent ones). It will probably consist of both antibiotics (ironically) and a standard colonoscopy preparation (regardless of whether the FMT delivery method is via colonoscopy or enema).
5. Colonoscopy delivered FMT to the Ileum is still best practice as far as I know (this was pioneered by Prof Tom Borody). Then there is a succession of follow up enema FMTs. Nine of them (one a day for nine days after the colonoscopy) in some recommendations. It is just a personal belief, but having had a couple of cracks at FMT (no pun intended) I find the donor is the most important thing, not the number of repeats. Based off an n=1, I’d say two or three follow ups on successive days works just fine if the donor is any good. I mention this because regardless of how it is done, follow up enema FMT is about as much fun as you’d imagine.
6. Get the right gear to get the job done (for enema FMT). There is a bit involved here. A clinic that does FMT would probably supply everything. Otherwise there is a bit of a list of stuff for doing it yourself. For the amateur enthusiast, a good nose clip is worth its weight in gold. The professionals don’t even use them. And that was before people started losing their sense of smell from Covid-19.
7. Follow the right process (for enema FMT). Again, there is detail here and a clinic providing FMT should have their own process. One point that stands out is that when mashing things up with the saline, I believe best practice is still to use a zip lock and do it manually. Blender aeration oxidises bacteria, which isn’t optimal. I even know of a blender malfunction in a clinic that had predictable, undesirable results. Regardless of how the FMT is prepared and made ready to go, you’ll still be doing the enema yourself. From experience, the act of enema delivery is the least demanding bit. It is the upstream and downstream materials handling that is the rough bit. Regardless, there isn’t a lot of dignity involved in enema FMT, but then again, neither is there with ME/CFS.
8. If you get a result, it is usually within 24 hours. The symptom relief can be significant, and across the board. However, in my experience, it doesn’t mean you are out of the woods. If you push things, you will still get PEM. In my experience, it will require far more effort to induce. Of course, that is dependent on the FMT having worked, but regardless PEM will still be there. Let things settle in and gradually increase your pacing window. Some people say they completely recover after FMT. I haven’t experienced that, but I have had the ~70% symptom improvement that is reported in research papers. Symptom improvement continually diminishes over time in my experience. But remaining better than when you started can last for years, particularly in regards to improved GI symptoms and avoiding dysbiosis. PEM and brain fog are a bit more of a mixed bag. Other people say FMT makes no difference to ME/CFS symptoms. I strongly believe that donor suitability is a big part of the equation, but that is just intuition and anecdotally based. I also suspect that the number of years you’ve had ME/CFS for is also a major contributing factor to an FMT working. That is, the longer you’ve had ME/CFS, the less chance you’ll experience “recovery” after an FMT. And, the biggest symptom improvement benefit seems to come from the first FMT process (as in, the first series of FMTs).
9. Get you microbiome scanned again. Complete the before and after microbiome picture. Any other data that you measure along the way (resting heart rate variability or whatever) would also be a good idea.
Hi Lono, I was submitting my comment at the same time you posted yours so I didn’t see this until now. Thank you for this detailed discussion of your experience with FMT, it is appreciated.
Re 2d. I’ve been of the understanding (from various sources) that immediate family are the better or best donors for FMT. Given they microbiome is seeded from the mother, makes decent sense as you would want to repopulate with same or similar species.
Thanks ManShadow. Regards 2D – I should state that this is just what I’ve heard talking to clinicians, and has no back up from research. It is just anecdotal based on cases, with probably some theorising mixed in. It sounds like your sources might be better.
Essentially, there are two factors regarding relatives that I know of. The first is diversity. One FMT practice recommended getting as many donors in the mix as possible for the greatest microbiome diversity. That is how the clinic produces their FMT “product” – many donors in one FMT. The second is that because of the ME/CFS genetic links, the microbiome of a close relative may have some degree of the same problems experienced by an ME/CFS patient.
I remember watching a popular science show years ago where they did speed dating based on smelling T-shirts provided on an anonymous basis. Apparently, your intuition around someone smelling good is linked to the “compatibility” of your immune systems. I don’t know how that relates to FMT, and I hope there isn’t an equivalent selection process. I suspect even the scientists and doctors at the forefront of microbiome research know of clinically relevant phenomena without having much of an idea as to why they occur (as yet).
My point is that I really don’t think anyone (myself included) has anything much better than hand waving arguments about donor optimisation. Donor exclusion, by contrast, is better understood in some ways (e.g. the donor screening tests), but not always. There was one article about a woman who became obese after having an FMT with her obese daughter as the donor. So in regards to relatives being better or worse for FMT in general, it is probably neither but actually depends on a heap of factors that are not well understood. I just avoid relatives as donors because of the ME/CFS genetic links.
I’ve got one other thought about casting as wide a net as possible for donor screening. Having the donor’s microbiome scanned might also be a good idea. When my microbiome was first scanned, I had some weird bugs I’d probably picked up through work and travel. There is no standard screening for these if they are obscure, they just popped up as part of the microbiome analysis.
I don’t know how knowledge has progressed in the last two years , but I was highly interested in gut microbiome stuff a few years ago and even tried some targeted hacking using the resources on cfsremission.com I had a swab test done of my gut biome, fed the data into the tool linked in that site and then did a bit of extra research so I wasn’t just relying on the one source. Used probiotics, prebiotics, certain whole foods, supplements, etc. All targeted at increasing useful species and decreasing supposed harmful species. Redid the microbiome test two times over the following few months and the results were really hard to draw any conclusions from. Symptoms didn’t change either (no increase nor decrease).
Didn’t get the anticipated results, but found out some handy info along the way such as a certain probiotic that gave me a really relaxed and warm feeling in my body. And there was also a lot of general knowledge I found interesting.
My lack of useful results put me off, but also the fact that the more I learned the more apparent it became that research is in its infancy and the high number of species in the biome, made me feel that any sort of useful understanding is a long ways off. 10 years at least. There also seems to be a lot of health practitioners out there that are IMO jumping on the bandwagon way too soon, so this contributes to a general misunderstanding among the public and that’s more of a peeve. I
I was also looking into DIY FMT and had a donor lined up and the relevant equipment ready to go. Just didn’t really get around to it in the end, I think I was grossed out by it but my conscious mind wouldn’t permit that fact at the time ?
“The gut may seem distant from the main source of action in chronic fatigue syndrome (ME/CFS) and fibromyalgia (FM) but more and more studies suggest that gut problems can affect everything from the cardiovascular system to the immune system to the brain.”
Hi Cort, it would be greatly appreciated if you would be so kind to strengthen the use of Myalgic encephalomyelitis in your correspondence and communications. As a decades long and now severe case ME sufferer who lives below the poverty line, I can attest to the continual denial of care under Medicaid, social services, and countless other areas due to the use of CFS. I have dropped it from my communications altogether.
I’d also like to add a word of caution to the use of Andrographis paniculata. Even though Andrographis has a long standing record of effective treatment, it can be stimulating and may cause anaphylactic reactions in some. https://selfhacked.com/2016/03/25/top-12-scientific-benefits-of-andrographis-paniculata-including-dosage-safety-and-side-effects/
Lastly, adding FMT as an effective healer to the discussion my benefit? FMT has its risks but I think it is worthy of consideration.
https://www.openbiome.org/about-fmt
Thanks Sumitra
“As a decades long and now severe case ME sufferer who lives below the poverty line, I can attest to the continual denial of care under Medicaid, social services, and countless other areas due to the use of CFS. ”
I certainly appreciate that myalgic encephalomyelitis is a better term than CFS. The problem is twofold: for my purposes search engines are more familiar with CFS and people who don’t know about ME probably know CFS so I insert it a couple of times into the blogs.
The bureaucracy responsible for Medicaid, social services etc. doesn’t know ME and I imagine that chances getting any support from them using that term are slim. In part this is probably because very little research has been published using the ME nomenclature – almost all papers use chronic fatigue syndrome or ME/CFS.
So while the ME term is much better the “logistics” of doing so make replacing the other terms with it problematic.
Thanks Cort, but your statement–
“The bureaucracy responsible for Medicaid, social services etc. doesn’t know ME and I imagine that chances getting any support from them using that term are slim.” has not been my experience, in fact, it has been the complete opposite, hence my initial post. Over the years I found myself consistently and immediately dismissed when using CFS, whereas ME has made people pay attention where they then will typically ask me the more important question of what ME is. They become seriously concerned as opposed to the very distinct, dismissive and “sighing” tone that CFS engenders. I have to take the time to educate them but it is well worth it and hopefully serves the greater good for others in need.
Thanks Sumitra,
My concern is that the evidence base for ME as ME is quite small but I can certainly appreciate that focusing on it would perk up a bureaucrat’s ears and provide a better entree than the term CFS. (As I noted I use “CFS” as little as possible and mostly for SEO purposes.)
Thanks for sharing your experience and I hope that others will have similar ones.
So where can I get me some Andrographolide and SsnB?
AG is readily available in supplement form in the U.S. and WebMD has prepared a section on it. Look it up on the internet and sources will pop up.
I don’t think SSnB is.
As a long term sufferer of CFS/ME, Fibro and Lyme diagnosis I first had my gut tested in 1998. This was in an Australian Chronic Pain Uni dept who had figured Gut Microbiome had a huge affect on these illnesses with a treatment protocol put in place.
I despair at the time it has taken to take this research further and don’t hold out much hope for this new treatment happening anytime soon.
That’s a long time ago and the gut is VERY complex and I agree it is taking a heck of a long time but we are learning more and more about it, some trends have emerged. Obviously, we need more money and many more researchers to do gut studies. It is encouraging that we can piggyback to some extent off of GWI studies and – the one I’m excited about – a fecal transplant study is underway in ME/CFS. Hang in there!
Gut: The number one source of Serotonin, my number one problem.
Plus: Moderna vaccine, now six months without relief.
They use the word Rare for side effects, that can mean 1/1k to 1/10k, that could equal 180k. It’s just numbers you know, to them anyway.
The intent of the covid-19 vaccine is not to prevent infection or the spreading of infection, only to prevent death and lessen it’s effects, per Fauci.
A 18 month old baby of fully vaccinated parents caught the vid, no they didn’t go anyplace recently. Stated “This virus will be seasonal”
Господи, помилуй (Lord have Mercy)
What a lie. Vaccination was indeed to prevent disease and spread. That was the suggestion from Fernando et al.’s original study https://www.nejm.org/doi/full/10.1056/nejmoa2034577 . Only 6 people were infected with Covid-19 after vaccination with Pfizer compared to 162 people with the placebo drug.
It seems that the vaccines are not working well. Israel is proof of that. Nor has it been proven that you get less sick if you are vaccinated. Most people didn’t get very sick from it.
Very annoying if this is true because I think most vaccinated people now feel cheated. Though they won’t like to admit it. Not to mention the mess you got inside. Fat globules with nanoparticles.
Pfizer just only 42% effective against Delta variant…..
New Study
https://www.businessinsider.com/pfizer-vaccine-efficacy-dropped-when-delta-became-dominant-study-2021-8?international=true&r=US&IR=T
For everybody how has taken Pfizer, would you take a vaccine 2 times for only 42% effctivity?
Not sure why the comment section has devolved into misinformation about Covid vaccines. Covid vaccines lessen but do not eliminate your risk of becoming a carrier of the new delta variant. But because they prime a healthy immune system to produce antibodies, they prevent the delta variant – which initially takes up residence in the nose and throat – from then migrating to and damaging the lungs and other organ systems. That’s why vaccines greatly reduce the risk of symptomatic infection, hospitalization, death, and (presumably) long Covid. Nobody I know who has been vaccinated feels cheated, except by the hordes of anti-vaxxers who refuse to get vaccinated, thereby fostering more viral mutations.
Personally ,I don’t feel cheated – I feel very grateful to get the vaccine. If more people had gotten the vaccine I would feel even better!
The 42% is against the possibility of being infected – not being hospitalized. The vaccines were never supposed to stop infections – they’re supposed to stop severe illness. They certainly do, however, reduce infectivity; that is, vaccinated people are significantly less likely to pass the virus on if they get infected than unvaccinated people. It appears that may be waning a bit.
The Isreal study which showed a drop in the ability of the Pfizer vaccine to thwart infections still found it was very effective at stopping people from getting really sick.
This is from a recent large SIngapore study.
https://www.news-medical.net/news/20210802/Study-shows-efficacy-of-Pfizer-BioNTech-and-Moderna-vaccines-against-SARS-CoV-2-delta-variant.aspx
That’s why, although I’m still double-masking – I’m very glad to have gotten the vaccine.
Hi Cort, why you still wear mask? You protected 🙂 I see the study. But also in the healthy population only 0.01 % of the people end up in a hospital. Israel is leading in the daily practice and ahead of the world, They demonstrate other different numbers. The doctors there warn that Pfizer is not sufficiently effective against the Delata variant.
In the original study by Pfizer, safety was investigated for only 2 months. I am curious what will happen in a year and after 5 years with vaccinated people. In india, the delta variant without mass vaccination is already on the decline.
How many hospitalized people are vaccinated in the US? And in Europe? They don’t know because they don’t keep track of it.
But let’s assume that vaccination helps to prevent serious illness from the Delta variant. Then I have bad news because the Lambda variant is resistant to the vaccines that are currently being used. So then we’re back to square one. https://www.forbes.com/sites/williamhaseltine/2021/08/10/it-is-time-to-pay-close-attention-to-the-lambda-variant-now-devastating-south-america/?sh=be132f54348e
Ron, please explain what you mean by serotonin being your main problem. Too much? Too little? Fluxuating?
Absolutely Too much Serotonin. After given SSRI’s+ in the belief that low Serotonin was the problem of my me/cfs, many things became intolerable. There is much written about the subject of excess Serotonin. One good source is Ray Peat.
Ron, another good source on serotonin is this article https://www.rolf-hefti.com/tryptophan-side-effects.html , which Ray Peat praised.
Peat has good company:
“To our knowledge, there is not a single peer-reviewed article that can be accurately cited to directly support claims of serotonin deficiency in any mental disorder, while there are many articles that present counterevidence.”
(Meaning, evidence of raised serotonin)
https://journals.plos.org/plosmedicine/article?id=10.1371/journal.pmed.0020392
Also:
https://www.bmj.com/content/350/bmj.h1771
You can find many more articles and research digging around.
– – – – – – – – –
Cases of eosinophilia-myalgia syndrome resulted from tryptophan supplementation.They blamed it on a toxic substances in the manufacturing process and banned its sale for some years. Interestingly, there have been case reports of the disease of individuals that weren’t even on the supplements and years later, cases still pop up.
It is a neurological disease also affecting muscles – sound familiar?
While not exactly the same as ME/CFS or FMS, there may be something relevant to learn here: excess tryptophan/serotonin/quinolic acid etc.
Also, eosinophils have a role in tissue remodeling, there are excellent recent studies on this, one specific in muscles stands out.
That means that wherever there is tissue damage, eosinophils can be recruited to start the regeneration process.
This certainly upends the notion that eosinophils are causing the damage to begin with, and therapies of steroids/immunosuppressants questionable, just as SSRIs are.
Be cautious of anyone suggesting that as an individual with ME/CFS or FMS, you have a ‘low’ serotonin problem, and hence would benefit from supplementing tryptophan or 5HTP etc.
A blood test is proof of little.
Where is serum tryptophan/serotomin coming from and going to?
Ron Davies mentioned that there is an initial rise in serum tryptophan and then it normalizes. And the metabolic trap hypothesis – it’s in immune cells. How do you measure tryptophan in immune cells?
Did you know that white/grey hair has a high content of tryptophan? May this be one way the excess is removed from the body, exiled to Siberia? Surely other substanves and process are invocled, this may be part of it.
I notice many with ME/CFS, FMS and hEDS have premature greying of hair. Or a sudden appearance at the onset of worsening of disease.
There is no misinformation. Only facts are presented. which are not pleasing to people who are fixated on vaccinations. Having an adult conversation is not possible with the obsessed vaccine advocates. There is never a substantive response when people are critical or start asking difficult questions to so-called scientists. You should not doubt otherwise you are against vaccination. Anti-vaxxers. Or even conspiracy theorists. In this way they ridicule and silence people with difficult questions. This is exactly what has happened with ME/CFS patients. Those same scientists say that this disease does not exist at all. The COVID-19 virus has never even been isolated. The gold standard. So how did the scientists develop the primers?
And where is the evidence that unvaccinated people cause mutations. All the mutations were already there. So your assumption still has to be proven and you can only say that when everyone has been vaccinated. The problem is that there is no longer a control group anymore. Even before there were vaccinations, many infections were a-symptomatic and very few people became seriously ill. Fact: In Isarel, up to 95% of new covid patients are fully vaccinated and become seriously ill. The number of IC recordings is increasing again. In addition, there are many examples in Europe in nursing homes where vaccinated people still die from Covid after vaccination. But enough. Back on topic.
Isn’t pyridostigmine bromide Mestinon? It is used for POTS especially if there are motility issues. And David Systrom is using it to help with PEM in ME/CFS.
If Gulf War Syndrome may be altered gut biome. Do you think that Systrom’s work also shows improvement after altering the gut biome?
I would not be surprised at all if when Mestinon works it improves gut motility which, in turn, could lead to better gut flora.
The link between gut microbiome and autoantibodies is a likely link in both FM and ME. Pathogens, xenotoxins (such as glyphosate and quaternary ammonium salts used in agriculture), food bactericides such as sulphites and nitrites and genetic predisposition possibly act together to cause dysbiosis and loss of tight-junction”. These could be accelerated in high sugar diets.
The link between FM and autoantibodies has been strengthened (even confirmed) by the recent research in UK and Sweden.
Four members of my family have significant gut dysbiosis which, in three, preceded the ME/FM. In my case I was mis-diagnosed with reactive arthropathy partly because of the massive diarrea following a “viral” infection. The fourth is inherited from his mother (Had ME during his pregnancy). However the fourth is significantly affected by xenotoxins.
The link between gut microbiome and autoantibodies is most studied in M.S. Such as : https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5845559/
https://pubmed.ncbi.nlm.nih.gov/31771976/
https://www.nature.com/articles/s41385-019-0192-y.pdf?proof=t
https://www.genengnews.com/news/gut-microbiome-influences-b-cell-and-antibody-repertoire/
Recent research suggests that a combination of b. subtilis and b. coagulans significantly reduced dyspepsia and ibs. These two bacteria are very prone to colony reduction due to antibiotics and xenotoxins leading to significant leaky gut. They are also prone to phage attack disabling them. I am unsure as to any link between a viral infection and effects on the bacteriome. However we do know that the gut microbiota influence viral infections.
The link between gut microbiome and autoantibodies is a likely link in both FM and ME. Pathogens, xenotoxins (such as glyphosate and quaternary ammonium salts used in agriculture), food bactericides such as sulphites and nitrites and genetic predisposition possibly act together to cause dysbiosis and loss of tight-junction”. These could be accelerated in high sugar diets.
The link between FM and autoantibodies has been strengthened (even confirmed) by the recent research in UK and Sweden.
Four members of my family have significant gut dysbiosis which, in three, preceded the ME/FM. In my case I was mis-diagnosed with reactive arthropathy partly because of the massive diarrea following a “viral” infection. The fourth is inherited from his mother (Had ME during his pregnancy). However the fourth is significantly affected by xenotoxins.
The link between gut microbiome and autoantibodies is most studied in M.S. Such as : https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5845559/
https://pubmed.ncbi.nlm.nih.gov/31771976/
https://www.nature.com/articles/s41385-019-0192-y.pdf?proof=t
https://www.genengnews.com/news/gut-microbiome-influences-b-cell-and-antibody-repertoire/
Recent research suggests that a combination of b. subtilis and b. coagulans significantly reduced dyspepsia and ibs. These two bacteria are very prone to colony reduction due to antibiotics and xenotoxins leading to significant leaky gut. They are also prone to phage attack disabling them. I am unsure as to any link between a viral infection and effects on the bacteriome. However we do know that the gut microbiota influence viral infections.
https://www.frontiersin.org/articles/10.3389/fcimb.2020.596166/full
If anyone can direct me to the effects of viral infection on gut bacteria I would appreciate it.
Sorry for the duplication in my post.
I know a lot about Gulf War Syndrome and exposures that may have triggered it. About nine months after the first Gulf War, our National Birth Defect Registry started receiving reports of birth defects in the veterans’ children. When I asked our advisory board of seven prominent scientists if we should create a special section of the registry questionnaire to collect data on exposures in these veterans, the panel enthusiastically agreed. We contacted the General Accounting Office to get a list of exposures in the Gulf. There were 31 categories of reproductive toxicants, i.e. an exposure that has caused adverse reproductive outcomes in animal or human studies. (Almost all exposures that can cause birth defects can also cause other health problems.) We added the new section to our questionnaire and began collecting data. It a short time, we found an increase in a very rare cranial-facial syndrome. We had quite a lot of national publicity about this, so I was invited to present our data to the Presidential Advisory Commission on Gulf War Illnesses and later to the Veterans Administration’s Scientific Advisory Commission on Gulf War Illnesses. A DOD study later found a tripling of the same cranial-facial birth defects in Gulf War veterans’ children born in military hospitals.
In order for an exposure to a male veteran to result in a birth defect, the causative agent is most often stored in their body fat. Our hypothesis was that this agent could be the pesticide chlorpyrifos that was widely used on blankets, camp perimeters and in numerous ways in the Gulf to control fleas, sand flies and other pests.
Chlorpyrifos is an organophosphate pesticide with a chlorinated structure. This means it can be stored in body fat. We even found an animal study that showed Dursban could cause the body to accumulate mercury.
This was all of interest to me because I had been exposed to chlorpyrifos for flea control in our home at the beginning of my ME/CFS in the early 1980’s. My symptoms mirrored those of Gulf War veterans.
Chlorpyrifos was removed from residential use in the early 2000’s. Some states have banned it use altogether.
I have both an elevated body burden of mercury and xylene which is a solvent used in the chlorpyrifos formulation.
If you have a toxic body burden and you exercise, get too hot, undergo severe stress, etc., you can start to dump these chemicals/heavy metals into your blood stream where they will cause havoc if you are deficient in part or all of the genes for methylation that would help break these down into harmless compounds.
This is why sudden weight loss or detoxification can be so dangerous.
Since these toxins can adversely affect your immune system, they can cause elevations in bacteria, mycoplasma and all kinds of herpes family viruses (EBV, HHV 6 a & b, Herpes Zoster, CMV, etc.) with all that entails.
I have a theory about how it could upend gut function. This involves the concept of haptens.
Hapten: In immunology, a molecule that is incapable, alone, of causing the production of antibodies but which can do so when fastened to a larger antigenic molecule called a carrier.
I believe, these toxins may cause gut problems when they attach to larger proteins like the gluten in wheat.
So what can you do? The problem becomes one of management and staying within boundaries of activity that don’t overwhelm your system with too many toxins at once. The other strategy is to bolster methylation so that you can handle the toxins that pass through. You may also need to suppress viral and bacterial reactivation, but this will never be the final answer as long as your body is contaminated.
Hasn’t green tea been shown to significantly improve the gut biome as well as tighten the junctions in the intestinal wall?
Manshadow, do you remember what probiotic caused you to feel relaxed?
Have some family members with anxiety, wondering if that might help.
I have used andrographis for years, with excellent results in recovering from viral infections and improving my sense of well-being…perhaps this study shows why! I’m going to take it more frequently (given that I haven’t been sick since the pandemic started) and see what happens!
Congrats and thanks for sharing your experience. I had never even heard of andrographis before this.
65 yr old female with fibromyalgia took all three covid shots. The first one no side affects that stand out. Second shot, vomiting and not wanting to eat for many days with diarrhea. Then booster which caused my whole body to tense up big time, diarrhea and not wanting to eat and endless acid reflux and burping for hours, poor sleep. Tried yogurt and sauerkraut but not really solving gastro issues. After three weeks the right side sort of backed off with tension beyond what fibromyalgia does. Then noticed all but the left knee area backed off with tight tension. Left knee got stuck and inflamed so badly I ended up having to use wheel chair and going to doctor. They took xrays, all fine. They then prescribed 800mg of ibuprofen for three days with food. That made a huge difference with the knee but also I found my whole body felt like BEFORE fibromyalgia. It has been 20 yrs and it was very obvious to me that this is what fibromyalgia is for me. This made me pause that my fibromyalgia was about a whole body inflammatory response. My bowels were improving too. Burping gone and I slept in for the first time in a long time and felt rested. For me this is an aha moment.
Years earlier I went to a young female managed care GP who was just awful and I told her I didn’t feel like myself. I thought maybe my hormones were off and looking back I now know I was going thru periomenopause. But this frustrated young GP who later quit passed me onto a therapist of all things. Maybe they knew something I didn’t on this. They talked me into using Paxil and said it was safe since I did not want to take anything that was addictive.
Soon after I noticed my arms aching and explained that to the therapist but she shrugged it off. Then I gained a lot of weight and she mentioned it but I wasn’t doing anything different. They didn’t understand the drug at the time since it was new but it turns out getting off of it is like getting off of heroin. Well they just kept upping my dosage since I was not feeling different or it wasn’t doing what they thought it should or I was caught in the web of bad medicine. I was on the maximum dosage of 60 mg and by that time I was sleeping thru the day. The therapist office would call me the day of my appt to remind me to come in, I was that out of it. I should not have been driving. I was not really able to make responsible decisions either. Finally someone decided this was a disaster after being on this for about 4 yrs and backed me off and then the therapist bails since she knows I am in for a hell of an episode of DTs and she makes out like I had made all this progress and I don’t need her. Not sure what the progress was other than me helping fill her monthly quota. She worked for Kaiser and has disappeared since. No one warned me of the withdrawals and probably hoped I would somehow not have them and they would get off the hook. At about 5 or 10 mg I got the DTs. Did not go back to them since they lied and inept and could not trust them. After weeks of serious DTs and all that goes with that I found I could not eat so many foods without significant gastro issues. Coffee was like battery acid in my stomach now. For a year after getting off of Paxil I had zapping sounds in my ears. My stomach was in a constant state of queasy. My brain felt fried. Also my whole body now ached big time and that was how I got fibromyalgia!
That was 20ish years ago I have lived with this condition ever since. Clearly I was inflamed all over which caused pain and we labeled it fibromyalgia, but once I took covid shots it cranked up my inflammation big time and I literally stiffed up all over with some serious inflammation which affected my stomach, colon and other organs. I literally had a storm of inflammation from the covid shots. They really should warn us to brace for this inflammatory storm and to take ibuprofen at 800 mg for three days with autoimmune issues. I still think we should take the shots but they way they did not prepare us for this was a sham because they did not want to give any ammunition for the anti vaxers to use. This was a fail and a bad decision.
I have been off of ibuprofen for four days now and I am now reverting back to the stiff fibromyalgia like before. Next steps: talk to my doctor about how often I can take big doses of ibuprofen to kind of give me a breather from the constant pain and poor sleep. Change diet once again.
I did try Paleo Autoimmune diet but my weight loss plateaued and it was not the entire answer. I do think the gut flora regulates so much and I do think that is what has caused my leaky gut and thus the inflammation all over. So many are selling an anti inflammatory diets and again I fear they miss the finer details with science like Paleo did. Cordain was not talking about gut flora at all but later decided to finally catch up. This is what happens with a sport medicine guy who was also training to be an optometrist decides he wants to be a researcher without the background and creds. It was a slipper slope for him and I can see why he finally retired and why so many distanced themselves from him since his science was rudimentary on it and half baked. I know since I was part of his so called autoimmune study that never really did much. No wonder he had such a hard time getting university approval, they already knew how he operated.
Alessio Fasano who is THE guy on the topic of celiac wrote a paper a few years back called the Leaky Gut and Autoimmunity. He believes that the answers for autoimmunity lies in the gut flora which is highly complex. He says all autoimmunity is cause by a leaky gut. If that is the case maybe they will have some sort of probiotic pill you take before we eat to shore up the junctions in our guts before we eat since I wonder if diet alone will fix it since gut issues can be caused by drugs and could be permanently damaged? Certainly the brain inflammation will have long term consequences too?
I think the problem is that funding for research for this stuff has been side lined over the decades. Instead the focus has been having professors get cozy with big pharma to sell them drug ideas to keep the conditions in play which is much more profitable. I do think big money does influence how universities operate and what they focus on and what is funded. Also if it is cured there is no way to really make it super profitable golden goose for any investors. The Microbiome Project finished many years ago, 2011? and we are not really seeing much come out of it. Lots of clues as to where we need to push on this but not seeing anything big coming from it for the big obvious group of 50 million with autoimmune in the U.S. alone. I read that big pharma makes more then the oil companies which is a ton of money. So the money is there the will do research this beyond immune suppressing drugs is not there. For me it was the drug companies that caused my fibromyalgia and maybe that is the reason they don’t want to research this, because the smoking gun may lie in their hands and the liability with all that would be astronomical?
Some do believe. For those who served in country in the gulf war. The US Veterans Administration (VA) has determined those with CFS, FM, IBS. it is considered service connected and eligible for compensation.