

Two chronic fatigue syndrome (ME/CFS) experts; Dr. Kaufman – an internist, and Dr. Ruhoy – a neurologist – began a more or less weekly Patreon channel called Unraveled: Understanding Complex Illness in December of last year. The Patreon broadcast provides the rare chance to see two experts who are deeply immersed in these diseases publicly dig into their many different aspects.
In an email, Dr. Kaufman spoke about their goal in doing the Patreon series – which is occurring at least once a week.
“Our goal, our reason for doing this, is to get the word out there and not just to patients but to their families and especially to other physicians. I am quite passionate about the desperate need to recruit more physicians to this work both for ME/CFS and the exploding epidemic of Long Covid. In addition to pulling/luring physicians into this work–which is incredibly challenging and rewarding–I want to help educate primary care physicians since they are–or should be–the backbone and foundation of healthcare in general and particularly for this patient population.”
Health Rising last covered Episode #3 – The “Septad” – a Treatment Roadmap for ME/CFS, POTS, Long COVID.
Please note that the following is attached to the beginning and end of every podcast.
Now we’re onto Episode #4.
Episode #4: Craniocervical Instability
What an episode this is! It’s quite possible there would be no discussion of craniocervical instability (CCI) in ME/CFS and related diseases without Dr. Kaufman. Jeff Wood – in the most remarkable display of self-diagnosis I’ve ever seen – started the CCI ME/CFS conversation off about five years ago.
Somehow Jeff – who was very severely ill at the time – came up with the idea that he had a condition that no one had connected with ME/CFS before. Not only that, but it was a rare condition afflicting the upper spine which (in his case) would require major spinal surgery to fix. Jeff, not surprisingly, struck out in his attempts to have doctors give his hypothesis a shot – until he met up with Dr. Kaufman.
Dr. Kaufman gave him the referral and the rest is history. Jeff had the surgery, fully recovered, and spread the news and now CCI, tethered cord syndrome, and other spinal issues (cerebral spinal fluid leaks, idiopathic intracranial hypertension, cerebellar tonsils) are part of the diagnostic algorithm for many ME/CFS experts.
Doctors have come a long way since Jeff and Jen Brea startled the ME/CFS communities with their remarkable recoveries from their severe ME/CFS. Please note, though, that while there have been some remarkable recoveries, some people have not done well at all with surgery, and some people have had much more moderate results. This is a work in progress.
Given that Dr. Kaufman and Dr. Ruhoy, a neurologist, have probably seen more CCI ME/CFS patients than any other doctor, this episode was a great opportunity to get it straight from the horse’s mouth. What more, really, could you want?
“Super Relevant” Problem
The episode started off with Dr. Ruhoy stating that they had both seen “many” of these patients, with Dr. Kaufman stating the condition was “super-relevant” and Dr. Ruhoy, a neurologist, noted that it was probably particularly relevant to patients who were house or bedbound and/or had problems with dysautonomia, and/or hypermobility.
CCI all revolves around the CO-CI or atlantooccipital joint. It’s a joint at the top of the spine which separates the skull from the vertebrae. It’s not just a separator, though, it’s actually part of the brainstem, the blood vessels that feed the brain, compartments of cerebral spinal fluid, and can be associated with low-lying cerebellar tonsils or Chiari malformation.
It’s clearly a densely packed piece of real estate in the body.
The Atlantooccipital Joint
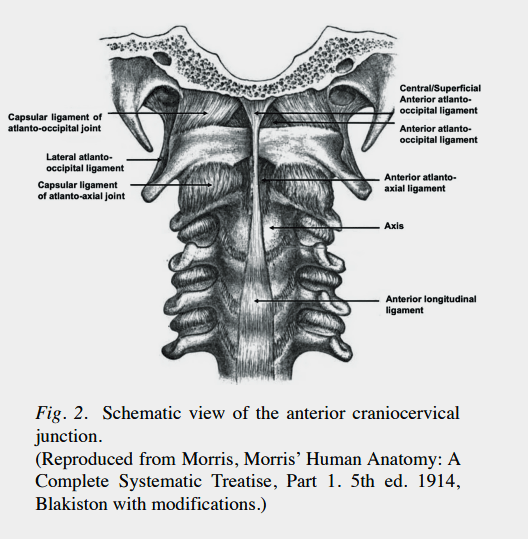
The atlantooccipital joint – The most mobile and complicated joint in the body. Note how it sits just above the vertebrae (from Kikuta_et_al_2020)
Dr. Kaufman offered up a picturesque view of the atlantooccipital joint. Humans, he noted have a very heavy brain sitting on a little neck. The brain is held in place by the most mobile joint in the body which allows us to turn our heads in all sorts of directions. (Jen Brea – another CCI patient – later recognized that her inability to turn her head to one side without sometimes severe symptoms was an indication that she had CCI). That great mobility arises out of 20 different ligaments twisting in and out of the CCI.
Information from the brain flows into the brainstem and then makes it into the spinal cord, and passes through an opening called the foramen magnum in the skull. Heavy head, easily damaged ligaments, tender spinal cord, intermixed with lots of bones – it is amazing things don’t go wrong more often.
The problem involves ligament laxity; i.e. the 20 ligaments in the area can no longer hold the skull in its proper place. Connective tissue problems, trauma (such as whiplash, from concussions), and infections can all degrade the ligaments and cause instability.
It was good to hear Dr. Ruhoy state that having CCI was “not necessarily a problem” at least so far as needing to have surgery, but then stated that since it’s an anatomical problem, the surgery is really the only way to correct the anatomy.
That’s not the total picture though. Reducing the inflammation that is attacking the ligaments to tighten them up can help. Still, CCI tends to be a progressive condition. Dr. Kaufman agreed that the challenge for them as physicians is “finding and diagnosing those patients before they have instability or CCI”, because although there are things they can “hopefully do to tighten the ligaments”, once anatomical instability is present, he “wasn’t sure that anything else will fix that”.
The whole subject of spinal surgery – which Dr. Ruhoy noted that not too many people were crazy about – was part of a “huge conversation” that Dr. Kaufman said he had with his patients. You can’t “lift the head (back) up” to where it should be simply with exercise or therapy”.
Symptoms include things like “my head feels too heavy”; and symptoms that flare when the head is in a certain position, some people may hold their head differently on their neck. Dr. Ruhoy said she’d looked for a straight line across their ears. An off-kilter line doesn’t mean they have CCI, but in the presence of symptoms, it is suggestive. (More on how to diagnose CCI in the next episode.)
One thing that happens in CCI is that the low end of the brainstem – which contains neural pathways that can affect just about any function in the body – gets impacted by the skull.
The Knotty Question – to Have Surgery or Not – and If So, When?
The surgery is a fusion between C0 and C2 – not something that Dr. Ruhoy would, as a neurologist, have as her endgame, but it’s the most effective means of correcting CCI right now.

Dr. Bolognese appear to be their surgeon of choice.
Dr. Kaufman noted that there is a spectrum. Some patients have some “unstableness”. They may have postural orthostatic tachycardia syndrome (POTS), dysautonomia, and hypermobility but they are still functioning and can hold down a job. His job is to keep them functioning, reduce inflammation, and tighten up their ligaments.
Others are not so functional but not bedbound, often not able to work, have more severe POTS, have more severe mast cell activation, they are doing sort of OK – and may be heading towards surgery, but they try to avoid it.
Then there’s the profoundly disabled, mostly bedbound, group. Dr. Kaufman noted all the drugs in the world, all the titrations, all the treatments for mast cell, bacterial overgrowth, their autoimmune problems – which can otherwise work in their case – do not get them better – because he cannot fix a damaged brainstem.
Given that it’s much harder to get these very ill patients to have this surgery done, the question is: do they have patients who are not bedbound do the surgery before they get so ill that they have more trouble getting the surgery done, recovering from it, etc.?
Dr. Ruhoy said that she was seeing a good response from injection therapies, but since they don’t correct the underlying connective tissue situation, she didn’t know that it would obviate the need for surgery at some point.
Stating “It’s a huge challenge”, Dr. Kaufman stated for the past 40 years he’s done anything possible to have his patients avoid surgery, but in this instance, he’s done a complete 180-degree turn on this. “Professionally and personally, it’s very challenging” for him since he knows how major this surgery is. But the fewer the comorbidities, the less bedbound, the better their muscles work, and the better their prognosis post-surgery.
With regard to his bedbound patients – Dr. Kaufman said he has changed his tune. He is now “convinced” that if a patient is bedbound, they have CCI – until is ruled out – it is that common in bedbound patients. In these patients, instead of going for the low-hanging fruit (mast cell activation, infection, POTS) first, and then looking at CCI, he’s immediately investigating whether they have CCI, checking out traction, looking for physical therapy – because he’s pretty sure that’s where they’re headed.
Dr. Ruhoy agreed. At Mt. Sinai, as with Dr. Kaufman, they go after the mast cell, POTS, etc. because that helps prepare for the surgery and recovery.
First Step – Manual Traction
If the imaging indicates it’s safe, Dr. Ruhoy and Dr. Kaufman try to do manual traction at home. Not only is getting a cervical MRI for his bedbound patients difficult, but is almost always normal in the typical radiology reports. (Special kinds of imaging are needed to distinguish CCI and allied issues).
Plus, the imaging results at these levels are not always in sync with the symptoms. (This is actually a well-known issue with imaging of all kinds.) Ruhoy has seen a “remarkable” clinical response to traction at home in people with either normal or borderline cervical issues.
(As an aside, Ruhoy noted that in almost all the MRIs, she sees a loss of lordosis (curvature of the spine) and degenerative issues (cervical disc disease) – even in relatively young people).
Dr. Kaufman agreed that regardless of the imaging results, the “money” for him regarding diagnosis is in the “powerfully revealing” response to traction. He prefers hands-on traction but noted it can be difficult to do. Dr. Ruhoy actually prefers home traction as you can control the weight.
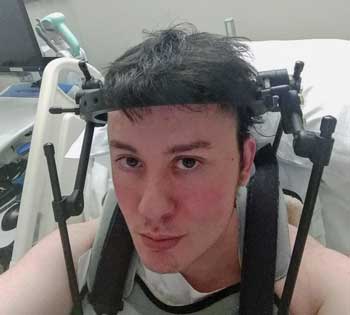
Jeff found that a halo stabilized his spine and improved his symptoms prior to his surgery with Dr. Bolognese (Not all CCI/AAI patients require a halo).
Second Step – Invasive Cervical Traction
If the manual traction proves helpful, the next step is to do invasive cervical traction (ICT) – something that only Dr. Paolo Bolognese – clearly their go-to surgeon – does in the U.S. It’s a vital step because it also helps with prognosis; a good result from the invasive cervical traction means patient is a good candidate for the surgery – and is an important part of pre-surgery planning.
Since Dr. Bolognese is doing imaging at the same time the traction is underway, it also gives him guidance regarding the surgery. At every increment of change in the traction, Bolognese takes pictures and asks about symptoms.
The ICT simulates the effects of the fusion and Dr. Bolognese uses the results of the fusion to find the sweet spot for the surgery. Dr. Ruhoy said she wouldn’t do a CCI surgery without it.
The Gist
- Dr. Ruhoy and Dr. Kaufman’s Patreon series continues with Episode 4: Craniocervical Instability (CCI) – the inability of the joint at the top of the spine – the most mobile and complicated joint in the body – to keep the skull in place – allowing it to settle on the brainstem and potentially causing virtually every symptom in the body.
- It’s no surprise that they covered this topic so early. Both consider it “super-relevant” to ME/CFS and related diseases, and Dr. Kaufman was the first ME/CFS doctor to consider it and ultimately uncover it.
- After Jeff Woods and Jen Brea’s successful surgeries for CCI, tethered cord syndrome, and other spinal issues (cerebral spinal fluid leaks, idiopathic intracranial hypertension, cerebellar tonsils), it became part of the diagnostic algorithm for many ME/CFS experts.
- The problem involves ligament laxity; i.e. the ligaments are no longer able to hold the skull in its proper place. Connective tissue problems, trauma (such as whiplash, from concussions), and infections can all degrade the ligaments and cause instability.
- Since CCI tends to be a progressive condition, the challenge for doctors is finding and diagnosing those patients before they have instability or CCI because although there are things they can “hopefully do to tighten the ligaments”, once anatomical instability is present, nothing but surgery will work.
- The subject of spinal surgery is part of a “huge conversation” that Dr. Kaufman said he had with his patients. Unfortunately, you can’t “lift the head (back) up” to where it should be simply with exercise or therapy.
- There is a spectrum. His job with patients with some “unstableness” who may have postural orthostatic instability syndrome (POTS), dysautonomia, and hypermobility, but are still functioning and can hold down a job, is to keep them functioning, reduce inflammation, and try and tighten up their ligaments.
- Others who are not so functional but not bedbound, often not able to work, have more severe POTS, have more severe mast cell activation, are doing sort of OK – may be heading towards surgery.
- Regarding the profoundly disabled, mostly bedbound, group, Dr. Kaufman noted all the drugs in the world, all the titrations, all the treatments for mast cell, bacterial overgrowth, their autoimmune problems – which can work in their case – do not get them better – because he cannot fix a damaged brainstem. Unless he is shown evidence to the contrary, he assumes that all bedbound patients have CCI, tethered cord syndrome, or both. With these patients, he immediately investigates whether they have CCI.
- Given that it’s much harder to get these very ill patients to have this surgery done, the question is: do they have patients who are not bedbound do the surgery before they get so ill that they have more trouble getting the surgery done, recovering from it, etc.?
- Using at-home traction or manual traction to begin to assess whether CCI is present is much more revealing than doing standard imaging (which is mostly useless). Reducing symptoms via these methods is a powerful indicator that CCI may be present.
- The next step is invasive cervical traction – done in the U.S. only by Dr. Bolognese. Not only can it be extraordinarily revealing but it also helps Dr. Bolognese plan the surgery, if necessary.
- Calling it a “miracle”, Dr. Ruhoy said that when she’s been in the room during an ICT, the response almost brings tears to her eyes.
- Dr. Kaufman noted that if you have more than CCI – as many patients do – you need to take a global approach and fix the mast cell problems, the POTS, the autoimmune issues, etc. to get well. Failed CCI stories may have occurred because these other things were not taken into account.
- Both Kaufman and Ruhoy agreed that alternative methods such as injections can only temporarily help and are extraordinarily expensive.
- Kaufman said he’s “almost at the point” where if he has a patient with POTS, MCAS, and the other parts of the septad, he’s convinced that if he doesn’t aggressively do things to strengthen their connective tissue – that patient is going to need CCI surgery at some point.
- Some treatments may be coming. Dr. Ruhoy said she has seen patients respond to peptide and stem cell therapies (Kaufman agreed).
- Next up – diagnosing CCI.
Dr. Bolognese is looking for resounding symptomatic changes as the traction – which lifts the head off the brainstem – occurs – as well as structural changes. Ruhoy and Kaufman have seen significant structural changes as a result of the ICT – but not significant clinical changes – and vice versa. In those cases, Bolognese usually repeats the test in 3-6 months.
Dr. Kaufman said to physicians who are skeptical of invasive cervical traction (ICT) – just watch a few videos – it is a “miracle”. Dr. Ruhoy said that when she’s been in the room during an ICT, the response almost brings tears to her eyes. People’s faces change, she said.
Kaufman said that during ICT, he’s seen patients state that they didn’t know they had trouble with their vision but all of a sudden they could see clearly, or their hearing clears up – they can hear clearly now, or think clearly.
In the Septad (the seven main interacting features of these diseases), everything interacts with everything. Kaufman, noting the negative reports regarding CCI that sometimes circulate on social media, asserted that you can’t expect CCI to fix everything. If you have more than CCI – as many patients do – you need to take a global approach and fix the mast cell problems, the POTS, the autoimmune issues, etc. as well.
Almost everyone he’s sent for a fusion has also ended up having a “tethered cord”. He’s also seen things like “venous compression syndrome” and Dr. Ruhoy noted that “eagle syndrome” can also be found.
Since these are different surgeries and both sometimes need to be done, the question arises what to fix first? Dr. Ruhoy said that doing the CCI first can make the tethered cord worse and vice versa. (Releasing the tethered cord can create a pull on the CCI and fixing the CCI can impact the tethered cord). The treatment approach is clearly evolving. Dr. Kaufman said that at first, Dr. Bolognese always did the more difficult CCI surgery first. Now he’s doing the tethered cord first.
Alternative Approaches
Dr. Kaufman asked Dr. Ruhoy an important question: have you seen any patients that you were sure needed CCI receive clear benefits from alternative alternatives such as injections? Dr. Ruhoy said yes, but the benefits were short-lived. This is because the injections can provoke a mast cell reaction that needs to be managed.
In the end, Dr. Kaufman and Dr. Ruhoy came down rather hard on injections – stating that they can cause tens of thousands of out-of-pocket dollars – and at the end of the day, while they can temporarily help, they aren’t fixing the problem. Dr. Kaufman compared the situation to having a flat tire. If you’re driving your car and you have a flat tire, you cannot fix that tire unless you jack up the tire. Injections, in other words, don’t jack up the tire; i.e. tighten up the ligaments.
Again it was back to: when is the optimal time for surgery? Ruhoy said that for young patients who are still functional, she tells them they’re a good candidate. She strongly recommends it. Dr. Kaufman asked: how do we identify patients who are at risk for surgery at some point. He outlined three groups of patients:
- Patients with connective tissue disorders such as hypermobility.
- Patients who have chronic inflammation (mast cell activation syndrome, POTS, leaky guts, infection) who do not have connective tissue disorder.
- Patients with both – Kaufman said he’s “almost at the point” where if he has a patient with POTS, MCAS, and the other parts of the septad, if he doesn’t aggressively do things to strengthen their connective tissue – that patient is going to need CCI surgery at some point.
Some treatments may be coming. Dr. Ruhoy said she has seen patients respond to peptide and stem cell therapies (Kaufman agreed), and she thinks the answer may ultimately be there.
Dr. Kaufman reiterated that his goal is to find ways to avoid the surgery. The problem is that most alternatives are often experimental, not FDA-approved, never covered by insurance, etc.
More on Craniocervical Instability
- Craniocervical Instability, Neurosurgery and M.E.: Just the Facts, Please – An Editorial by Jeff Wood
- Jeff Woods Mechanical Basis website
- Jen Brea’s Amazing ME/CFS Recovery
- Health Rising’s Craniocervical Instability and Spinal Issues Poll







Hi Cort. Theres an incorrect word in this sentence – instability:
“Dr. Kaufman noted that there is a spectrum. Some patients have some “unstableness”. They may have postural orthostatic instability syndrome (POTS)”.
Great article though. Wish there were more surgeons and it was more affordable!
Turned POTS into an instability syndrome (LOL). Thanks!
My connective tissue improved immediately after my spinal CSF leak was repaired (leaks damage/weaken connective tissue). I was bedbound for nearly a year but a blood patch and the heaviness, inability to hold up my head, and spike in heart rate when turning my head were gone. I would love to see anyone getting evaluated for this surgery to first be evaluated by a leak specialist.
(But I’m also THRILLED they’re looking more closely at this!)
I agree with you, Melissa. It is always best to start with the least restrictive approaches. When a neurosurgeon seems so sure that people need surgery, the saying that comes to mind is, “When all you have is a hammer, everything looks like a nail.” The most holistic approach would also include evaluating a person’s stress levels, as stress is a major cause of inflammation. In the case of this article, it seems the best approach would be to address the other issues first and save the surgery as a last option.
I have EDS and had terrible problems with neck instability. In 2016 I began the Cusack protocol and within weeks of taking the fractionally distilled aloe vera juice, I no longer had that bobblehead feeling or needed to wear a cervical collar. Quite amazing, really. My other joints also became much more stable and I don’t get massive flares when I accidentally bump a wall or kick a curb.
I still have issues with almost daily subluxation of C1 & C2, triggering migraines, but thankfully, I’m married to a chiropractor and he takes care of that problem. Not a permanent solution by any means – I’m still homebound and disabled – but I no longer have to spend half the day in bed. I’m also in no shape, mentally, physically or financially, to fight for appropriate tests and surgery.
The Cusack Protocol (specifically the aloe) is definitely one of the most important tools in my arsenal.
Thank you, Cort for your excellent work! You are so appreciated.
Thanks for telling us about the Cusack protocol, Kristen! It’s good to hear about alternatives. Let’s hope we can find some more permanent answers to the ligament issue.
I don’t understand this diagnostic pathway at all. I was diagnosed by Dr. Bolognese with “mild to moderate at best” CCI and told to do neck exercises and conservative treatments since traction didn’t relieve my PEM and I’m not a candidate for surgery. So, it’s basically a dead end for my case of ME??? I’m housebound and disabled, but my CCI isn’t a path towards a cure?? So bizarre.
Apparently it’s not for you. Your path leads elsewhere. Hopefully, it will get uncovered soon.
Thank you Cort 🙏
This article helps to explain why Alexander Technique is the only thing that’s ever helped me with chronic fatigue and generalised pain (which I now understand to be myofascial).
The whole of AT centres around the pivotal point of posture: how the heavy head sits on top of the spine. If this is wrong, nothing else will be right: throwing the spine out for a start — which then affects everything else.
AT teaches a sense of balance through interoception: increased internal awareness of one’s “use” of the body: and how to let go of tight (contracted) muscles that maintain misuse, generating pain and fatigue from the unremitting demands on mitochondria in muscle cells.
I now think of my own chronic fatigue as mainfestation of Repetitive Strain Injury (RSI) throughout my body — but focused on the back of my neck where it meets my skull.
My current self-defined task is to keep stretching the back of my neck while letting my head rotate to bring down my chin, while letting go of ALL the other habitually tensed muscles in my face, scalp, shoulders, arms, torso, legs, feet…
It’s also fascinating to learn about the multi-function fascia that (from what I now experience) seems to have seized up too: and to think how many habits I need to drop. Like holding a mobile phone & typing on it (what I’m doing now), playing Spider Solitaire — all keeping my hands/ arms / shoulders / upper body rigid, exacerbating habitual tension held in my jaw.
I discover new areas of internal strain every day (or rather, night) as the internal “letting go” becomes more extensive, revealing even deeper layers of toghtness a nd contraction.
And I think it’s probably time to have more Alexander lessons, to have someone to talk to about it and observe the changes I can’t see.
“Dr. Kaufman reiterated that his goal is to find ways to avoid the surgery. The problem is that most alternatives are often experimental, not FDA-approved, never covered by insurance, etc.”
Dr Kaufman should probably look into Alexander Technique. And into Feldenkrais, as an apparently similar movement therapy.
Alexander Technique is a great idea in my book. Kaufman doesn’t believe efforts like this would affect the ligament laxity but they could help resolve tension in the neck/head area which is such an area of tightness and pain. Anything to help out that area would be great.
Alexander Technique helped me for a few years but it never “took” for very long. I finally ran out of money for it — and lost patience for my practicioner’s blaming me for its not working.
Now I’m worked with an MD Spine Specialist, an excellent PT, and a pain doctor whose 4 pain injections in my neck enabled me to get out of locked position.
AT is great for the short term, but it doesn’t correct anything. And you have to see a practicioner pretty much every week to keep things “in line.” I think they have a glimmer of the problem, but don’t have the solution.
I’m no longer a fan.
I’m glad you agree that Alexander Technique is worth a try. It has definitely helped me. It’s worth adding that one-to-one hands-on lessons need to be from a qualified teacher (Society of Teachers of the Alexander Technique STAT in the UK, sorry I don’t know the qualifying body in the US or elsewhere).
It can be useful to start in an introductory small group (I did a day-long workshop with two other beginners) but it then needs to be one-to-one with a teacher.
And it’s not cheap (but worth every penny). It also cannot be learnt from books: though there are some interesting books about it, worth reading.
And it takes least half a dozen lessons to get into it properly (though some benefits can be experienced immediately by some people): maintaining moment-to-moment awareness BETWEEN lessons too– or it’s a waste of time and money doing them at all!
AT has been described as “remapping the body onto the brain”: installing new sensorimotor neural circuits that come to feel “normal” the more they are practised, replacing the old dysfunctional circuits that used to feel “normal”.
Just getting the head-neck relationship right has effects that ripple through the whole body — but we often have a variety of other bad habits too.
Good luck to anyone who tries this.
I’m now progressing to myofascial release (a form of massage therapy) that seems like a good complement to AT — for the seized-up parts that AT cannot reach!
Always cones down to tissue type. Cci is downstream of that. Just looking at Jeff, he has that typical eds pallor.
We’re so far up the creek if regenerative medicine can’t help
Or… maybe this doctor is wrong about you! You know your body, your symptoms, your exact history, etc. better than anyone else so if you strongly feel CCI is very likely the source of your problems, don’t let one doctor’s opinion stop you from pursuing answers. CCI is so complex that it is very easy to be missed or written off as “mild” when maybe in actuality you do have a severe case that could be the cause to all your problems! that’s why this whole process sucks. You really have to be persistent and advocate for yourself every step of the way. Get a second opinion from one of the other known CCI experts after getting all the necessary proper imaging (DMX, upright MRI, and some of these neurosurgeons also like you to have a specific type of CT scan protocol done where you just need to have a neck and head ct scan done where you rotate your head all the way to left and hen all the way to the right. Once you have these imaging tests done, you will have visible (and measurable) evidence of whatever is happening in your cervical skip me and skull base. Then you will have your answers. You will have peace that either that doctor was right and you don’t have any CCI or associated problems, OR you will see for yourself that you indeed DO have problems and at what exact level of your cervical spine… and then you can go forward with finding the best doctor for you, equipped with the evidence to share and discuss with the proper neurosurgeons. You could even go back to this same doctor with the imaging evidence and if he doesn’t have an awful ego, he may re-evaluate you given the new evidence you have
I have Ehlers-Danlos Syndrome so as a super researcher, CCI, in my world view, has almost always been associated with EDS/hypermobility. I am greatly amused that the ME/CFS community (or at least certain doctors) have co-opted CCI as cause and effect for many of the issues that ME/CFS people have–things like POTS, MCAS etc. which are also so prevalent in EDS. So, fatigue, is also super common in hEDS, but PEM, not as much. EDSers describe ‘spoon theory’ where they only have so much energy every day, but not all of them have the day or days after crash like those with ME/CFS.
I frequently ask myself, is my fatigue from ME/CFS or EDS? Or a combination? I do have PEM, but not as severe as some. So who really ‘owns’ CCI, and all these symptoms? One is a genetic connective tissue disorder and the other, most likely a post viral illness.
Where these things start and where they end is anyone’s guess. These disorders seem to be part of a vast spectrum. We are starting to see some doctors like Kaufman and Ruhoy break out of their silo’s and branch out. I imagine we’ll hear much more about the connections between these disorders and the connective tissue and mast cell and other problems that bind them together as the series goes on.
Dr. Peter Rowe from Johns Hopkins Hospital is famous in the EDS community as one of the first to make these kinds of connections in the mid 1990s.
Another condition which manifests much like CCI is Chiari Malformation (adopted by the EDS community as one of their co-morbidities). It’s when the brain drops into the spinal cord, especially when a person is standing. Unfortunately, to diagnose it an upright scanner is needed. Many a sufferer is overlooked because when they are laying flat on an MRI, the brain is in a more normal position.
Both CCI and Chiari are thought by many to come from the wobbly nature of connective tissue which is a hallmark of EDS.
Behold the vast expanse of these kinds of problems which bedevils most doctors! My last visit to Stanford is where one of my doctors confirmed my comment that people like me with multiple issues with overlapping symptoms (and few confirmed treatments) are the worst kind of patients to have.
Connective tissue, connective tissue, connective tissue – found at that joint, the blood vessels, gut lining, muscles, etc. – it’s everywhere!
Even in the teeth (bone) as my mouth full of dental work can testify!
Connective tissue/fascia (or is it “fasciae”?) popping up so much in these latest entries you could do a blog about it some time! Check out this Arte documentary on fascia with English subs: https://m.youtube.com/watch?v=Owd3_JrAseo Would be great to have a fascia specialist join the ME/CFS train.
that you have to be in an upright scanner is extremely useful information!
I wish my neurologist was aware of it.
I’ll pass it on.
Thank you!
All interesting and well but almost 6 years later and still no evidence for the connection CCI >ME. What these surgeries actually do. No evidence for most of the things mentioned in this article…
Yes, some people seem to have a positive response but many do not. For a substantial group it has been a downright disaster.
Instead of telling skeptical MDs to watch a video maybe there finally should be studies published to actually show some evidence so we can prevent any further harm caused by these surgeries.
There are many theories about what causes ME. Maybe for some this could be a thing, but that does not mean we can just publish articles and promote surgeries without mentioning the fact that there’s a lack of evidence base and the amount of harms caused by the surgeries. That’s in my opinion really irresponsible!
Important letter on the subject: https://drive.google.com/file/d/1J86TnhvHRA29zlihgG9jiGAlTAQ_nFU-/view?usp=drivesdk
Yes, there should be studies – of course! I’m reporting on what the doctors are saying and yes, some people have been harmed – and hopefully Kaufman and Ruhoy will explore that as well.
Thus far, they clearly have found that these surgeries have been helpful and are promoting them for certain patients. That suggests that in the main they have found them to be quite helpful – and we need to figure out which people are likely to be helped (the healthier ones for sure) and for which it’s not a good option.
You made a good point, though and I added this to the blog
Hi Cort,
Thank you for adding that part to the blog. However it still doesn’t mention that there is a lack of evidence base for many of the things that are being said in this article. This is all/mostly based on clinical experience and opinions and that isn’t (always) the most reliable. My personal observation, including from some of my friends who underwent these surgeries, is that they aren’t that helpful and on the long run harmful. On top of that you’re fused for life. There’s no way back! We need to do everything to prevent any further harm. I don’t think these articles help to prevent them. In my opinion it only makes it worse. It needs a lot more critical reporting If you decide to write about it.
Anil, yes clinical experience is what Kaufman and Ruhoy are basing their podcast on. Many of these approaches are so new that one wouldn’t expect a study yet. But doctors who are skilled at such a level to, in good conscience, work from clinical experience is a step in the system eventually producing more solid knowledge such as studies. In this case, Mike Van Elzaker at Harvard/MGH and his team are doing such a study now, with a 7T MRI. I don’t think it is so much about the treatments – craniocervical fusion in particular – as it is about the physiology which links CCI to ME/CFS. So the science is catching up, and for Van Elzaker he places the Vagus nerve etc at the center of his theories about the etiology of ME/CFS.
And for what it is worth, every person we know well who has had a CCF (n=3) has had major improvements. Usually there are other things to track down, and folks can still struggle, but no regrets – especially from those who are so sick that a breathing/feeding tube is in play and who can then no longer have to suffer in that way. This n=3 includes one of the earliest patients. CCF for ME/CFS hasn’t been happening for long enough (5 years for patient 1) for anyone to know what happens in the long run – that’s certainly a concern. But know that for many this has been a life saver. Also, the possibility of the procedure not being of benefit is exactly why Kaufman and Ruhoy say they wouldn’t want to go down this road without the Invasive Traction test. I don’t have a link to one, but if you can find a video of that test you would start to see why Kaufman and Ruhoy are such “fans”.
That’s a good point – that they require a positive invasive traction test before going further and then Dr. Bolognese uses the results to guide his surgery. I guess we would have to know if others were as rigorous.
Traction is maybe indeed a good measure, but again no evidence. Really it’s not much work to publish a couple case studies for example to be scrutinized. That’s shouldn’t have to take almost 6 years.
We had 2 severe ME patients here in the Netherlands at the beginning who had some small improvements and relapsed. No traction in Spain at the time but we hear it from people who are patients from dr. B. as well.
Anyways, everyone needs to decide for themselves but this subject needs a lot more critical reporting than this current blog and previous articles have done in my opinion. We are critical of the harms caused by other (behavioral) treatments. We should be here just as much. I don’t see a reason for any double standards.
It’s a knotty subject for sure and I hope we will hear more from Kaufman and Ruhoy on success rates, and what goes wrong when it doesn’t work. I really feel for people who have had this major, major surgery done and didn’t get better and even got worse. That is a tough pill to swallow.
right!!!
Studies are lacking, but you can hear plenty of stories, both positive and negative, in the MECFS brain/spine surgery group on Facebook, as well as a group devoted to Bolognese. Absolutely, people should look critically, but there’s more evidence available listening to patients. And of course Kaufman and Ruhoy have together had well over a hundred patients go through this. My son went from bed bound, not able to eat most of the time, complete darkness etc. to walking. Did need a tethered cord surgery and is still not fully well, but we do not regret his decision for a moment. These surgeons spend more time helping people and refining technique (e.g. Bolognese now does vascular decompressions) than publishing, but they do give talks including some numbers. I think your skepticism goes beyond what is warranted, if you are willing to look hard and talk to people enough.
Well, we have two respected doctors who have plenty of experience in this area. For me, I will take their word on it.
For now, we can’t do any better than that. God knows how long it will take for evidence-based studies on this procedure to show up – if they ever do. It’s possible they will NEVER show up. There are plenty of treatments for ME/CFS for which we have no evidence-base – other than doctor’s and patients experience.
What we really need to do is to identify how everyone was diagnosed, whether they had invasive traction tests done first, who did the surgery, what kind of shape they were in prior to doing the surgery, etc.
The problem is that it seems that they are pretty locked into their worldview at this point…everything always points back to this for them, which can influence the entire diagnostic process. I agree, it’s been long enough now for some case studies to have been published at least. I saw a leading EDS geneticist recently who was VERY disparaging about Bolognese in particular…stating unequivocally that once someone had this type of surgery from him, if it went wrong, no one else would be willing to attempt a repair. Given Bolognese’s reputation for washing his hands of patients after surgery, this is indeed a problem if things go south. These surgeries are very controversial in the field at this point and with the leading proponents unwilling to share their case statistics, it’s impossible to know how many are truly helped vs harmed. I suspect if the numbers were truly that good, they would be sharing far and wide though.
“silo’s”?? …But Cort, this is something Germans do! (saying this as a German :-)) there’s even a German expression for it – Idiotenapostroph (probably self-translating 🙂 – meaning inappropriate addition of apostrophes in sometimes hilarious places onto the German language due to confusion resulting from common exposure of Germans to English language spelling. But you’re American – I’m in awe why I increasingly see this phenomenon in English language posts – hope you don’t mind a little tease 🙂
After further investigation to my question of ME/CFS vs. EDS, I found this article;
https://www.frontiersin.org/articles/10.3389/fneur.2020.00828/full
Another example of ideas which are not quite connected because sharing of information is so disorganized.
Hope you see this as I am always suspicious that comments never get read after a blog gets ‘old.’
Eds is the start. It’s the tissue type where all this stuff starts.eds and m.e. , I think will turn out to be flavours of the sane disease.
Connective tissue predisposes you to mast cell activation, which degrades already weak tissue, pots kicks in.body goes into shutdown to try and protect a failing body. Mitos shut down to protect the body, hence the fatigue.
I hope they find a way with crispr technology to heal us as I don’t fancy this surgery
I am in Queensland australia.
I believe I have cci and frayed spinal cord.
Would my neurologist know of these conditions and how to treat…
Waiting anxiously,
Glenys
Hi Glenys – I don’t know how well these conditions are known in Australia – they’re not that well known here – but the next Patreon episode we cover will be on diagnosis. Hopefully that will help. It’s Kaufman’s and Ruhoy’s goal, after all, to get this information out to doctors.
Thank you.
For approx. 3 weeks I have had a really weird HEAVY head which feels like it’s too heavy for ny body, and when I go to stand up I feel like I will fall over and everything is hard to do.
My neurologist said to cut my Entrostol tablet in half.
I an 80 and don’t want surgery.
Please help me.
Glenys
I’m in OZ too. You can try Macquarie neurosurgery & Spine https://mqneurosurgery.com.au/our-mission-and-values/#
I have no personal experience but know of someone who was diagnosed there with some of these problems.
I’m in OZ too. You can try Macquarie neurosurgery & Spine https://mqneurosurgery.com.au/our-mission-and-values/#
I have no personal experience but know of someone who was diagnosed there with some of these problems.
Hey Cort! As a retired X-Ray Tech that rendering of the anterior craniocervical junction took me aback, lol! What the heck are those horns ascending from the occipital skull?
Anyway, every time I read an episode of your newsletter I feel hopeful, which is immediately followed by the inevitable feeling of how discouraging this whole process is.
It’s been 14 years for me. Diagnosed with Fibromyalgia post medical trauma. I have hypermobility, but not ED. I have POTS and PEM, and am positive for Epstein Barr antibodies, but I don’t know when I had it. 5 autoimmune diseases and brain fog so thick I have to take notes when I read anything. Really appreciate your recap.
And there are SO many different approaches offering so many possibilities. It’s like an unfinished choreography that I’m dying to see if only someone would take charge. I guess the bright light on the horizon is Long Covid and all the research dollars that come along with a medically accepted chronic illness.
Not sure if anyone else is experiencing this, but doctors are so burnt out post pandemic and so over worked. My current PCP teaches at UCSF medical school and he told me in the entire graduating class only 2 students are going into Primary Care. He’s very worried about the future of front line care.
Very interesting about CCI. I have horrible problems with the craniocervical junction which in turn triggers migraine for me. I also am experiencing a “hardening” of my tendons due to my hypermobility.
Thanks again for another insightful newsletter Cort 🙂
“It’s like an unfinished choreography that I’m dying to see if only someone would take charge.”
Nicely said – lots of pieces out there. Looking forward to see how the dance of so many biological factors comes together! I think the good news is the doctors like Kaufman and Ruhoy are demonstrating the interconnections between these factors.
That illustration was from 1914!
I also like that analogy very much!
Thanks for highlighting these fantastic discussions between Dr Ruhoy and Dr Kaufman, I don’t think I’d have found them otherwise. I’ve gone back to the beginning and am watching all the episodes. I saw this one last week and I was riveted.
I think I’ve had slightly lax ligaments for years. I sort of have to pop things back where they should be, every now and again. I’ve also noticed that if I eat particular things, more problems arise.
A while back it felt like my right knee joint was becoming loose and unstable. My hips can click in and out a bit and more worryingly my jaw and neck has become crunchy at times. I believe that this may be in connection to an increase in inflammation, related to different foods – probably sugar.
Anyway, I’m loving the Patreon series of chats. It’s so refreshing to listen to doctors talk about their patients and their work with such care and compassion.
I wish this was something I could investigate further but I’m now into the ‘elderly’ age range and any serious surgery would be way too risky. I remember when Whitney Dafoe was anesthetized and had the scans and this problem was ruled out, so no surgery. Highly disappointing. Thanks for sharing updates.
Pris, do you know if Whitney had the very specific scan for this condition and they just didn’t find it? You’d think his father would make sure. It is certainly very tricky.
All I know was that Jenn Brea was involved. They found a top doctor. The anesthesia was used so they could position him correctly. The results said it wasn’t for him. I was so hopeful for him when that was going on. All of this was online so I know no other details.
I didn’t know he had gotten checked out but it makes sense. Jen Brea is a good friend and, of course, she has a lot of experience in this area. Dr. Kaufman said until proven otherwise he’s assuming people who are bedbound have this – and now we have an otherwise.
Thanks again, Cort for a terrific report. As I’ve got older and worse, I have been speculating that I have CCI and perhaps the other events that go with it. Certainly, my head often feels as if it’s about to fall off. Bending over and trying to, say, wipe the floor is lethal for me, as is sweeping, even a little bit. I get a pressure in the head and spine and other symptoms and they take days to ‘get over’.
Next time, could you ask these doctors what kinds of movements and activity might make the symptoms worse? Also, more detail about the symptoms, eg, tingling in the feet and legs. I wonder how this relates to the vascular problems you have also posted about.
I have no chance of getting an official diagnosis and it would be at least good to have more certainty. I am also in Australia and there is virtually no mention of this here and certainly not by medical professionals that I have heard of.
I am aware of the case of a woman around 40years who had the symptoms of ME/CFS who had the surgery in the US and is hugely improved, even doing a lot of running, still gets exhausted but is greatly improved.
I think we’ll get a full overview of the symptoms in the next podcast. If it’s not easy – but not impossible! – to get a diagnosis in the States – I imagine it’s more difficult elsewhere. Spreading the word, though, is what these podcasts are all about.
I wish this was easier – the last thing I would want to consider is spinal surgery but it’s also casting a light on connective tissue problems and inflammation – a good thing.
Looking forward to the next instalment, Cort, thanks.
I’m also reminded here of Peter Rowe’s work which gets into this area, although I haven’t seen him mention CCI as such. He’s mentioned by Nany B.
His speculations should really be tested: somewhat technical, in this para of his leg lift study, in which attempts to bring together a number of areas involved in movement in ME/CFS and its consequences:
Biomechanical and physiological considerations with SLR
found here: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0159386
Yes, indeed his neuromuscular strain work seems to fit right in with all this.
https://www.healthrising.org/blog/2014/07/08/unrestrained-dr-peter-rowe-neuromuscular-strain-chronic-fatigue-syndrome-mecfs/
There are different directions of instability. For example, vertical and horizontal. I had vertical instability, so being upright was difficult. I could counteract upright positions by laying down for a couple days or applying a light manual traction using my hands for a couple minutes. One activity that is hard for people with CCI is riding in a car. If you are mild enough, PT might get you more stability but it’s hard to find knowledgeable people. There is a good article about PT for CCI authored by Susan Chalela if you are interested.
An interesting thing to me is you see many elderly people with extreme curve to the neck ,yet still active.bi look normal but am up the kyber
Instead of “bending over” try bending your knees instead, going down with your head still balanced squarely on top of your spine. It can be very tough on the knees to begin with, but they get stronger the more they are used.
I have cranial instability. Along with my jaw falling out on one side, my crashing to the ground from weak ankle ligaments, and the lolling head, giddiness from head movement. have ME … and I have sustained injuries to the upper neck as well. Seeking medical help failed for probably the usual reasons of being in uncharted territory with this area of health intervention … alternative remedies were researched. My husband came across the use of creatin for athletes … and I take a little every day with remarkable results. …… The reason was that in cases of patients who have both ME as well as joint hypermobility, it was found in a study .. that the cells use available creatin as an energy source. This creatin is then not available for ligaments. ………………………….. My hair is thinning likely from taking creatin .. .. but my jaw started dropping out of its socket each time when I stopped taking the creatin. Each time I resume the creatin, the problem is rapidly resolved. With this intervention I am getting by with all the loose ligaments. I have to be very careful with my head ..as its instability, and compromised condition is evident.
Wow, Anne! Is that creatine you are taking?
This is such an interesting topic! I have CCI and am looking into treatments these days. Surgery is not an option for me, so I have to try alternatives.
I have kyphosis, forward head posture and a round back. Also, a bit of a duck Butt. I watched many videos on YouTube with exercises for kyphosis and the physiotherapists all said, that the round back causes the forward head posture. They all say, that there is no point in doing neck exercises, if the whole body posture is wrong. The neck adapts to the rest of the body.
I feel like the right approach is very relevant for exercises and I am still looking for it. I think relaxation of muscles is super important, because cramped up muscles cannot strengthen. I only do relaxation exercises at the moment.
Deep breathing is important for posture, too.
I have been doing breathing exercises and embodiment exercises, like body scan and progressive muscle relaxation and am noticing that some areas of my body are very cramped up. The pelvic floor and hip area is totally cramped up. I am trying to relax these muscles now. The pelvic floor is important for the posture of the whole body. It spans between the bottom of the spine and the pelvic bone.
Maybe a bit more holistic approach than surgery can help, too, at least sometimes? If the whole body is cramped up and in bad posture, surely this could affect the neck.
On phoenixrising, this thread is from someone, who got major improvement from neck massage, back and hip exercises and more:
https://forums.phoenixrising.me/threads/alternative-non-surgical-possibilities-for-addressing-cci-aai-or-other-serious-neck-issues.63041/
A true chiropractor who comes recommended by patients might help with posture?
Thank you Cort for your great reporting and summary.
Best wishes!
I was diagnosed with ME/CFS and Lyme back in 2019 (I contracted Lyme via an emergency blood transfusion in 2014). I saw improvement after Lyme treatment, but still had significant symptoms. An MRI revealed several issues with my neck and in 2021, I was diagnosed with CCI by a chiropractor (Ontario, Canada) who specializes in Atlas Orthogonal Adjustments. He was mentored by Dr. Rosa in New York, who is an expert in his field dealing with concussions (google him). My CCI is a result of a major car accident in 1998 and my neck was never treated. I was on my way to becoming bedbound with ME/CFS, but after 2 1/2 years of receiving Atlas Orthogonal Adjustments, I am much better and I am heading back to work after being off for 6 years! These adjustments have literally saved my life! The only downfall for me is that the adjustment doesn’t hold, which means that my symptoms do return but they are mild compared to what I was dealing with before. I go every two weeks for the adjustment and I couldn’t be more grateful. I know that surgery will be inevitable, but my goal is to put it off for as long as I can or until this condition is actually recognized in Canada.
Congratulations for finding something Tammy and thanks for passing that on 🙂
I think this is all interesting but I would not do surgery after hearing some surgery horror stories in the Facebook group where people discuss this exact issue and have ME/ CFS. My question is – how many people have messed up necks or backs, CCI but no ME/CFS symptoms? I imagine a lot. And then you have to ask- what’s the difference?
I remember from Jeff’s and Jen Brea’s cases that they were atypical for CCI; i.e. the ME/CFS CCI is different from other types of CCI.
Hmmm. Also, there is a woman on IG that was big in that group, helped people to read their X-rays that they posted. I guess she got really into learning. She said on IG or a blog she wrote (forgot where), that one day someone posted their wife’s neck X-ray and apparently it was a mess but she didn’t have cfs or I think any major issues. The woman then decided to get into brain retraining and is doing a lot better. Just sayin! @Already_healed is the IG she has links to her story. But I still think the CCI, back issue is interesting. I have scoliosis and know a lot of other people with CFS that also have scoliosis. I think maybe it comes down to allostatic load but i don’t buy that it’s the main answer for ME/CFS, even the bed bound people.
Is there any tie-in of all of this with migraine and atypical or headache free migraine?
“Our goal, our reason for doing this, is to get the word out there and not just to patients but to their families and especially to other physicians.”
With that primary goal in mind it’s confusing that they chose to lock their message behind a paywall on patreon.
All I can think is that if you want to really get the word out you need to get on a platform that many people use, and of, course, Patreon does charge for its services. In the end, though, while it would be great to have it for free, it’s still an incredible opportunity in my book for so many of us – who do not have access to ME/CFS experts – and even for those who do (and only have quite limited access) and for doctors – who can easily afford it – to learn from two of the best ME/CFS experts out there. I hope the doctors are signing up.
Agreed.
Not everyone who is bedbound with severe M.E. has CCI. I was a patient of both of these wonderful doctors. Dr Kaufman and Dr. Ruhoy. Unfortunately, neither was able to help me. One treatment actually caused me harm. They are both good people and well-intentioned. I have tried everything under the sun in every dimension for the last decades. Bedbound for many years. It took over a year to explore the CCI issue. I have now completely ruled out CCI. Regenexx is an alternative to surgery, but was told by the Dr. that I do not have CCI and even if I did, it does not cause the majority of the severe M.E. symptoms. So, this article stuck out to me because it is not true for what I have experienced on my journey.
Thanks for sharing your experience Seastar and good luck finding something that works!
this is truly insane.
Thanks for covering this topic, Cort. I had CCI for years following viral Meningitis. The symptoms were extremely difficult and disabling—migraines triggered by lifting something 5 lbs, craning my neck, reaching for something. Basically I couldn’t move my spine without triggering migraine. And even being upright and straight was problematic—mega brain fog as in couldn’t remember close friends names. I could go on and on about the disabling symptoms and difficulties getting a diagnosis. I went 15 years before getting diagnosed by Bolengnese, Henderson and Patel who all diagnosed me with CCi, Basilar Invagination, cranial settling and Chiari Malformation. I’ve always been hypermobile and around the time of getting CCI diagnosis, a geneticist diagnosed me with EDS. During this time I had mild fatigue which I now get was mild CFS/me. After my first fusion (CO-C3) all the migraines disappeared and did the difficulty thinking and speaking upright. Also I could barely swallow before surgery. Afterwards no problem. About six months after surgery my fatigue became way, way worse. I have probably about 4 decent hours/day. I’ve been diagnosed with CFS/me and have lawful PEM. Reactivated EBV, pots etc. So in my case CCI was not clearly the cause of fatigue. It’s more of an EdS collagen breakdown in my spine (also has had CFS leaks, have Tarlov cysts and FMD in vertebral arteries). I think this was triggered by the meningitis plus mega psychological stress at the time. Even though I have moderate to severe CFS/ME I am much less disabled post CCF. I had to get the fusion revised in May because the other did not hold and the instability symptoms had returned. Post surgery they are gone. Yes, surgery is a last resort but I wish I’d had mine a lot sooner. It’s hard to undo all the damage of years of brain stem compression and lack of CSF flow from Chiat (my tonsillar herniation was 9mm) and corrected itself after fusion. I’m so so grateful for my surgeries. Not a panacea clearly. I really appreciate the awareness you and the podcast doctors are bringing to the problem.
Chairi not spell checked Chiat
Why is it still unclear that collagen disorder/EDS/whatever you want to call it is behind all of these conditions due to multi-mechanistic and synergistic pathophysiologies? Lax vessels and ligaments, autonomic neuropathy, and probably many other undiscovered mechanisms that all drive cerebral hypo-perfusion. Majority of us have EDS along with another autonomic function hamper
Range of motion after surgery > https://www.youtube.com/watch?v=mV1-Tv-xMOo